Save Time & Money and Take the Stress out of OIG Exclusions Screening
- Make your life easier and save hours on manual exclusion checks!
- Helps you maintain compliance with federally funded healthcare programs.
- Helps prevent potential costly Civil Monetary Penalties.
- Batch Screen against OIG Exclusions, SAM Debarments, & all State Medicare Provider Termination Lists at once.
- Get a comprehensive Exclusions Report.
Just $25 / 100 Providers Screened
No registration or user account required
How Exclusions Screening Works

One: To use our Batch Exclusion Screening service, upload your list of NPI numbers in either Excel or text format.
Two: Provide your email to receive a link to the Exclusions Report, and then click Start.
Three: Click the download report link in the email to open the payment page. The price is based on the number of providers uploaded and screened.
The Exclusions Report automatically downloads after payment, which includes details for any OIG Exclusions, SAM Debarments, or State Medicaid Terminations found, ensuring you have the essential information needed to help protect you from potential Civil Monetary Penalties.
Benefits & Why It Matters
Monthly screening of new hires, existing employees, and contractors for OIG Exclusions, SAM Exclusions, and all State Medicaid Exclusion Lists is a compliance requirement for many healthcare organizations.
Providers excluded by the OIG or terminated by a State Medicaid Agency cannot participate in federally funded healthcare programs, including Medicaid, TRICARE, and the Children’s Health Insurance Program (CHIP).
Additionally, a provider whose billing privileges have been revoked by the Centers for Medicare & Medicaid Services (CMS) or any State Medicaid Agency is prohibited from participating in Medicare.
- Batch screening helps you maintain eligibility for federal programs.
- Batch screening reduces manual administrative work.
- Batch screening helps you avoid costly Civil Monetary Penalties.
Learn More about why you need to screen both OIG Exclusions and SAM Debarments.
Screen OIG Exclusions, SAM, and all State Medicare Exclusions Lists all at Once
Our Batch Medicare Exclusion Screening service checks providers against all major Federal & State exclusion databases, including:
- OIG Exclusions List of Excluded Individuals and Entities (LEIE)
- All State Medicaid Termination Lists
- SAM Debarments (SAM.gov)
- FDA Debarments
- FDA Clinical Investigator—Disqualification Proceedings
- CMS Medicare Opt-out Affidavits
- NPI Deactivation List
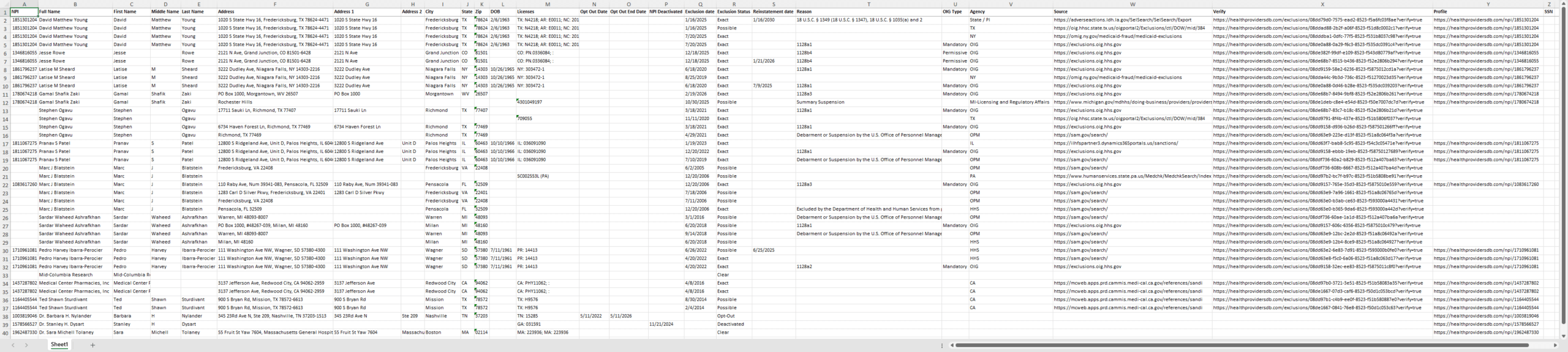
Comprehensive Exclusions Report
The Batch Exclusions Report includes:
- Full Name, First, Middle, and Last Names
- Full Address, Address 1, Address 2, City, State, Zip
- NPI Number and NPI Deactivated Date
- License Numbers
- Medicare Opt Out Affidavit Start and End Dates
- Exclusion Date, Reason, and Reinstatement Date
- Exclusion Status of Clear, Exact, Possible, Reinstated, Deactivated, Opted-out
- OIG, SAM, or State reporting Agency Details
- Plus, links to the Exclusion Source Data and Verification Page.
Frequently Asked Questions
Compliance: The Office of Inspector General (OIG) mandates screening to prevent fraud, abuse, and patient neglect.
Financial Risk: Hiring an excluded individual can result in substantial Civil Monetary Penalties (CMPs) and repayment obligations.
Requirement: 42 CFR Part § 455.436 Federal database checks require all Medicare Advantage Plans, all State Medicaid Programs, and all Medicaid Managed Care Organizations.
Healthcare Providers & Facilities: Hospitals, nursing homes, home health agencies, clinics, and physician practices.
Personnel: All employees (clinical and non-clinical), medical assistants, nurses, and administrative staff.
Contractors & Vendors: Third-party billing & coding services, ambulance services, and medical equipment suppliers.
Leadership & Support: Board members, managers, owners, and volunteers.
According to the OIG’s Special Advisory Bulletin issued in May 2013, the OIG recommends that healthcare organizations check their employees and contractors against the LEIE monthly.
42 CFR Part § 455.436(c)(2) Federal database checks states to “check the LEIE and SAM no less frequently than monthly.”
Monthly screening is mandatory in at least 14 States, while many others strongly recommend that providers screen employees and vendors against their State lists and the LEIE monthly.
Healthcare organizations must conduct OIG exclusion screening for all individuals and entities that provide items or services payable by federal health care programs.
This requirement applies to anyone whose work supports services reimbursed by Medicare or Medicaid—whether those services are provided directly or indirectly.
Individuals who must be screened may include:
Physicians, nurses, and clinical staff
Billing and coding personnel
Administrative and management staff
Medical equipment suppliers
Transportation providers
Pharmacy staff and pharmacists
Third-party contractors and vendors
Basically, if an individual’s role contributes in any way to federally reimbursable services, that individual should be included in your OIG exclusion screening and Medicare exclusion monitoring process.
Furthermore, the OIG has emphasized that civil monetary penalties are most likely when excluded individuals provide essential services to patient care.
Learn more about who needs to be screened for Medicare Exclusion.
